Introduction
Have you ever heard someone say they have fatty liver disease and wondered what that really means? Many people are surprised when their doctor tells them they have Grade 1, Grade 2, or Grade 3 fatty liver after an ultrasound. But what do these grades actually mean?
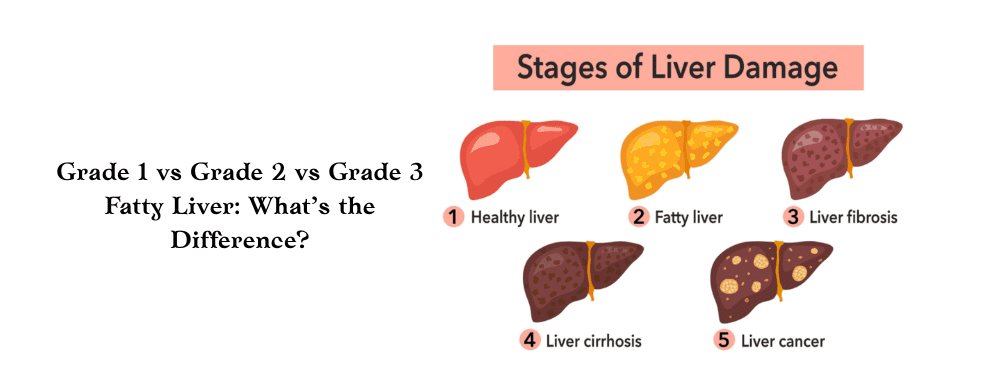
Think of your liver like a filter or a sponge that cleans your blood and removes toxins from the body. When too much fat builds up inside this sponge, it starts to lose its ability to work properly. Over time, the liver may become inflamed, damaged, or even scarred.
Fatty liver disease is becoming extremely common today due to unhealthy diets, obesity, diabetes, and sedentary lifestyles. The good news is that in the early stages it is reversible. However, if ignored, it can progress to serious conditions like cirrhosis or liver failure.
In this article, we will clearly explain the difference between Grade 1, Grade 2, and Grade 3 fatty liver, their symptoms, causes, diagnosis, treatment options, and when you should consult the best liver transplant surgeon in India.
Dr. Neerav Goyal is a renowned liver transplant specialist in India, known for advanced liver surgery, transplant expertise, and exceptional patient care.
What is fatty liver disease?
Fatty liver disease occurs when too much fat accumulates inside liver cells. Normally, the liver contains a small amount of fat, but when fat exceeds 5–10% of the liver’s weight, it becomes fatty liver disease.
There are two main types:
1. Non-Alcoholic Fatty Liver Disease (NAFLD)
Occurs in people who drink little or no alcohol.
2. Alcoholic Fatty Liver Disease
Caused by excessive alcohol consumption.
NAFLD is now one of the most common liver diseases worldwide, affecting millions of people.
Why Fat Builds Up in the Liver
Fat accumulation in the liver usually happens due to metabolic problems. When the body cannot process fat efficiently, excess fat gets stored in the liver.
Common Causes Include
-
Obesity
-
High cholesterol
-
Diabetes
-
Insulin resistance
-
Sedentary lifestyle
-
Poor diet (high sugar & processed foods)
Imagine your liver like a warehouse. When too many fat packages arrive and none leave, the warehouse becomes overcrowded.
Understanding the Grading of Fatty Liver
Doctors classify fatty liver disease into three grades based on how much fat is present in the liver.
These grades are usually detected through ultrasound imaging.
The Three Grades Are
-
Grade 1 – Mild fatty liver
-
Grade 2 – Moderate fatty liver
-
Grade 3 – Severe fatty liver
Each grade represents progressively increasing fat accumulation and potential damage.
What is Grade 1 Fatty Liver?
Grade 1 fatty liver is the mildest stage of the disease.
In This Stage
-
Small amounts of fat accumulate in liver cells
-
Liver function is usually normal
-
Most people have no symptoms
Key Features
-
Mild fat deposition
-
Minimal liver damage
-
Usually reversible with lifestyle changes
Common Causes
-
Obesity
-
High sugar intake
-
Lack of exercise
-
Early metabolic syndrome
Good News
Grade 1 fatty liver can often be completely reversed through:
-
Weight loss
-
Healthy diet
-
Regular exercise
What is Grade 2 Fatty Liver?
Grade 2 fatty liver indicates moderate fat accumulation in the liver.
At This Stage
-
Fat deposits increase
-
Liver may become slightly inflamed
-
Symptoms may start appearing
Possible Symptoms
-
Fatigue
-
Mild abdominal discomfort
-
Weakness
-
Slight enlargement of the liver
What Happens Inside the Liver
The liver starts showing structural changes, and the risk of inflammation increases.
If untreated, Grade 2 fatty liver may progress to fibrosis or cirrhosis.
What is Grade 3 Fatty Liver?
Grade 3 fatty liver is the most severe stage of fatty liver disease.
At This Point
-
Large amounts of fat cover the liver
-
Liver function may become impaired
-
Inflammation and scarring may begin
Symptoms of Grade 3 Fatty Liver
People may experience:
-
Severe fatigue
-
Abdominal pain
-
Nausea
-
Weight loss
-
Liver enlargement
Possible Complications
-
Liver fibrosis
-
Liver cirrhosis
-
Liver failure
-
Increased risk of liver cancer
In advanced cases, patients may require treatment from the best liver transplant surgeon in India if the liver becomes severely damaged.
Key Differences Between Grade 1, 2, and 3 Fatty Liver
| Feature | Grade 1 | Grade 2 | Grade 3 |
|---|---|---|---|
| Fat accumulation | Mild | Moderate | Severe |
| Symptoms | Usually none | Mild symptoms | Noticeable symptoms |
| Liver damage | Minimal | Moderate | Significant |
| Reversibility | Easily reversible | Reversible with treatment | Difficult but manageable |
| Risk of complications | Low | Moderate | High |
Symptoms of Different Fatty Liver Grades
One tricky part about fatty liver disease is that many people have no symptoms for years.
Possible Signs Include
-
Fatigue
-
Abdominal discomfort
-
Unexplained weight loss
-
Weakness
-
Loss of appetite
In Advanced Cases
-
Jaundice
-
Swelling in legs
-
Fluid in abdomen
Risk Factors for Fatty Liver Disease
Certain lifestyle and health factors increase the risk of fatty liver.
Major Risk Factors
-
Obesity
-
Diabetes
-
High cholesterol
-
High triglycerides
-
High blood pressure
-
Poor diet
People with metabolic syndrome are particularly at risk.
How Doctors Diagnose Fatty Liver
Doctors use several tests to diagnose fatty liver disease.
Common Diagnostic Tests
1. Ultrasound
Most common test to detect fatty liver.
2. Liver Function Tests (LFTs)
Check liver enzyme levels.
3. Fibroscan
Measures liver stiffness and fat content.
4. MRI or CT Scan
5. Liver Biopsy
Used in complex cases.
Early diagnosis is important to prevent disease progression.
Treatment Options for Fatty Liver
There is no specific medicine that cures fatty liver completely. Treatment focuses on removing the underlying cause.
Common Treatments
-
Weight loss
-
Blood sugar control
-
Cholesterol management
-
Exercise
-
Healthy diet
Doctors may also prescribe medications to manage associated conditions like diabetes or cholesterol.
Lifestyle Changes That Reverse Fatty Liver
The liver has an amazing ability to heal itself.
1. Lose Weight
Losing 5–10% of body weight can significantly reduce liver fat.
2. Exercise Regularly
At least 30 minutes of exercise daily helps burn liver fat.
3. Eat a Healthy Diet
Focus on:
-
Fruits
-
Vegetables
-
Whole grains
-
Lean protein
Avoid:
-
Sugar
-
Fried food
-
Processed food
4. Limit Alcohol
Alcohol accelerates liver damage.
When Fatty Liver Becomes Dangerous
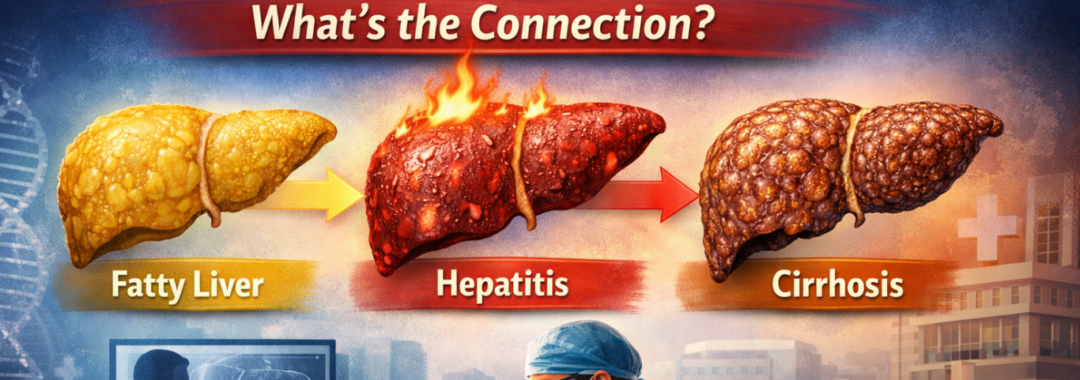
Fatty liver becomes dangerous when it progresses to:
-
NASH (Non-Alcoholic Steatohepatitis)
-
Liver fibrosis
-
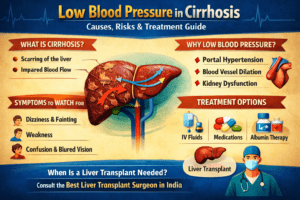
Cirrhosis
-
Liver failure
Cirrhosis can permanently damage the liver and may require a liver transplant.
This is when consultation with the best liver transplant surgeon in India becomes essential.
When to Consult a Liver Specialist
You should consult a doctor if you experience:
-
Persistent fatigue
-
Unexplained weight loss
-
Abdominal pain
-
Abnormal liver test results
-
Ultrasound showing fatty liver
Early treatment can prevent severe complications.
Can Fatty Liver Be Completely Cured?
Yes, especially in the early stages.
Grade 1 fatty liver is often completely reversible.
Grade 2 fatty liver can also improve with proper treatment and lifestyle changes.
Grade 3 fatty liver may require long-term medical management, and in rare cases advanced treatments including liver transplant.
The key is early detection and lifestyle correction.
Conclusion
Fatty liver disease is becoming increasingly common, but understanding its stages can help prevent serious complications. Grade 1 fatty liver is mild and usually reversible with healthy lifestyle changes. Grade 2 fatty liver indicates moderate fat accumulation and requires more attention to diet, exercise, and medical monitoring. Grade 3 fatty liver is severe and may lead to serious liver damage if not treated properly.
The good news is that the liver is incredibly resilient. With the right habits, early diagnosis, and proper treatment, many people can reverse fatty liver and restore their liver health. However, in advanced cases where the liver becomes severely damaged, consultation with the best liver transplant surgeon in India may become necessary to explore life-saving treatment options.
Taking care of your liver today is one of the best investments you can make for your long-term health.
FAQs
1. Can Grade 1 fatty liver become normal again?
Yes. Grade 1 fatty liver is usually reversible with weight loss, healthy diet, and regular exercise.
2. Is Grade 2 fatty liver serious?
Grade 2 fatty liver is moderate and should not be ignored. With proper lifestyle changes and medical care, it can often be reversed.
3. Is Grade 3 fatty liver dangerous?
Yes. Grade 3 fatty liver indicates severe fat accumulation and may lead to cirrhosis, liver failure, or liver cancer if untreated.
4. How long does it take to reverse fatty liver?
With proper lifestyle changes, improvement may be seen within 3–6 months, though complete recovery may take longer.
5. When is liver transplant needed for fatty liver disease?
A liver transplant may be required if fatty liver progresses to end-stage liver disease or cirrhosis, and the liver can no longer function properly. Consulting the best liver transplant surgeon in India is important in such cases.