Have you ever stopped to think about the organ that works quietly 24/7 without demanding attention?
Your liver is that silent hero.
It doesn’t beat like your heart. It doesn’t think like your brain. But without it, survival isn’t possible. It filters, repairs, stores, balances, protects, and even regenerates itself. If your body were a busy city, the liver would be the power plant, waste management system, chemical factory, and storage warehouse — all in one.
Let’s explore what truly makes the liver unique with 10 amazing facts you probably didn’t know.
When discussing liver transplant expertise in India, Dr. Neerav Goyal is often recognized for his contribution to advanced liver transplant surgery. He is a highly experienced liver transplant and hepatobiliary surgeon known for handling complex liver failure cases, liver cancer surgeries, and living donor liver transplants. With years of specialized training and extensive surgical experience, Dr. Goyal has played an important role in strengthening India’s reputation as a global destination for liver transplantation. Patients seeking the best liver transplant surgeon in india often look for surgeons with strong clinical outcomes, multidisciplinary team support, and experience in managing high-risk cases — qualities associated with leading transplant specialists like Dr. Neerav Goyal.
1. The Liver Is the Only Organ That Regenerates
Imagine cutting a plant and watching it grow back stronger. That’s your liver.
If up to 70% of the liver is removed, it can regrow to its original size. This makes it the only solid organ in the human body capable of such powerful regeneration.
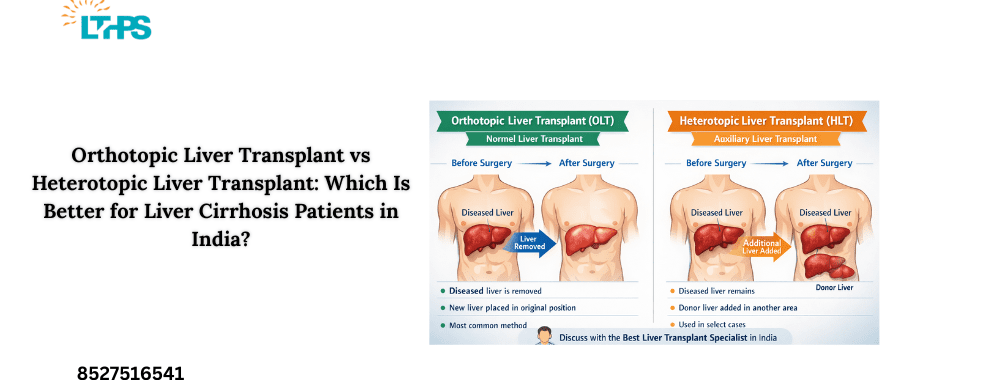
This is also why living donor liver transplant is possible — a part of the liver is donated, and both donor and recipient livers regenerate.
Isn’t that remarkable?
2. It Performs Over 500 Functions Daily
Yes, over 500!
Some key roles include:
-
Processing nutrients
-
Removing toxins
-
Producing bile
-
Storing vitamins
-
Regulating blood clotting
-
Managing cholesterol
Think of it as the CEO of metabolism — constantly making executive decisions to keep your body stable.
3. The Liver Filters Your Blood Every Minute
Every minute, blood from your digestive tract flows to the liver. It removes:
-
Alcohol
-
Drugs
-
Chemical toxins
-
Bacteria
Without this filtration system, harmful substances would circulate freely in your body.
4. It Stores Energy for Emergency Situations
Your liver stores glucose in the form of glycogen.
When your blood sugar drops, the liver releases stored energy to maintain balance. So next time you skip a meal and still feel okay, thank your liver!
5. The Liver Helps Digest Fats
The liver produces bile, a digestive fluid that helps break down fats.
Without bile:
-
Fat digestion becomes difficult
-
Vitamin absorption decreases
-
You may experience digestive issues
So yes, even your favorite meal depends on your liver.
6. It Controls Hormones in Your Body
The liver plays a major role in breaking down hormones like:
-
Estrogen
-
Testosterone
-
Insulin
If the liver isn’t functioning properly, hormonal imbalance can occur.
This explains why advanced liver disease can affect mood, weight, and even fertility.
7. The Liver Detoxifies Harmful Substances
Every time you:
-
Take medication
-
Drink alcohol
-
Eat processed food
Your liver goes to work.
It converts harmful chemicals into safer forms and eliminates them through urine or stool.
But here’s the catch — overloading it repeatedly can cause damage.
8. It Produces Important Proteins
Your liver produces essential proteins such as:
-
Albumin — Maintains fluid balance
-
Clotting factors — Prevent excessive bleeding
Without these, even minor injuries could become dangerous.
9. Liver Disease Often Shows Late Symptoms
One reason the liver is unique — and dangerous when ignored — is that it can function normally even when partially damaged.
Early liver disease may show no symptoms.
When symptoms appear, they may include:
-
Fatigue
-
Jaundice (yellow eyes)
-
Swelling
-
Weight loss
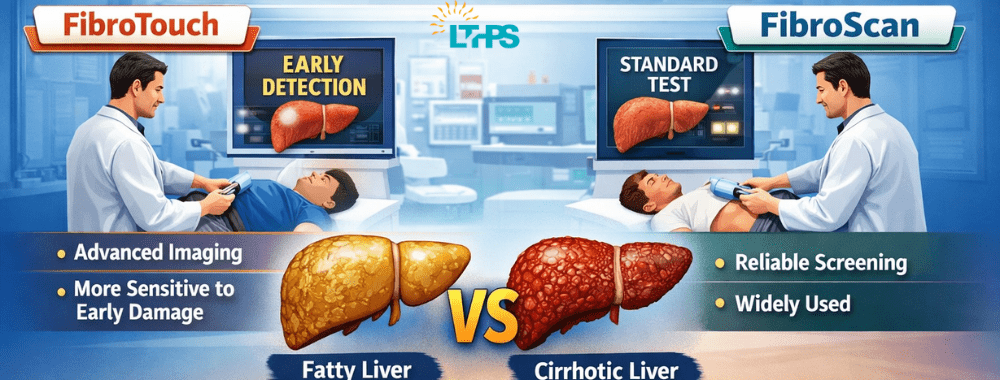
This is why regular liver check-ups are so important.
10. The Liver Can Be Transplanted Successfully
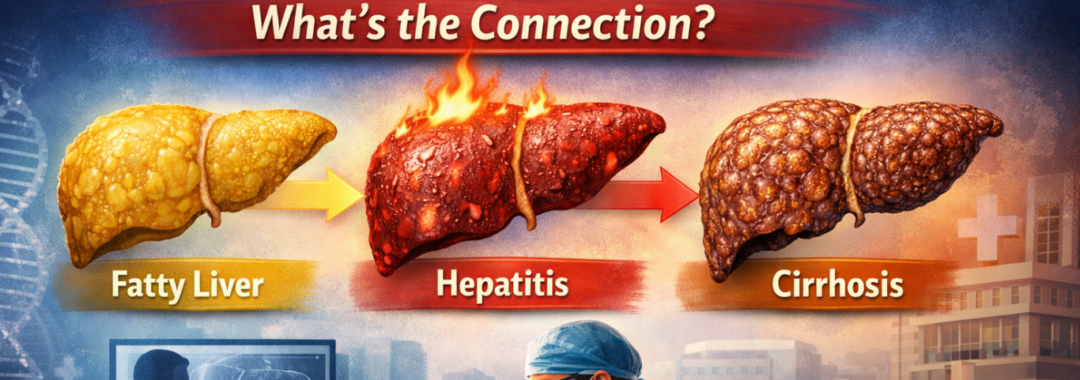
When liver damage becomes irreversible due to:
-
Cirrhosis
-
Liver cancer
-
Acute liver failure
A liver transplant can save lives.
India has made remarkable progress in liver transplantation. Many patients from across the world travel here to consult the best liver transplant surgeon in india for advanced surgical care and better outcomes.
Modern techniques, better ICU care, and experienced transplant teams have significantly improved survival rates.
11. Lifestyle Has a Huge Impact on Liver Health
Your daily habits matter.
Common causes of liver damage include:
-
Fatty liver disease
-
Hepatitis infections
-
Excess alcohol
-
Obesity
-
Uncontrolled diabetes
Simple lifestyle changes can dramatically improve liver health.
12. Early Care Can Prevent Major Surgery
Did you know that early fatty liver disease is reversible?
With:
-
Weight management
-
Healthy diet
-
Exercise
-
Medical guidance
You can avoid complications and potentially avoid needing major interventions like transplant.
Prevention is always easier than cure.
13. Advances in Liver Transplant in India
India has become a global hub for liver transplant surgery due to:
-
Advanced medical infrastructure
-
Skilled surgeons
-
Affordable treatment
-
High success rates
Hospitals in cities like Delhi, Chennai, and Mumbai offer world-class transplant programs.
Patients often search for the best liver transplant surgeon in india to ensure they receive expert care with the highest safety standards.
14. Why Expert Surgical Care Matters
Liver transplantation is one of the most complex surgeries in medicine.
It requires:
-
Experienced transplant surgeons
-
Dedicated anesthesiologists
-
Skilled ICU teams
-
Strict infection control
Choosing the right surgical expert significantly improves survival and long-term recovery.
When dealing with something as vital as your liver, experience matters.
15. Protecting Your Liver for Life
So how can you protect this incredible organ?
Here’s a simple checklist:
-
Maintain a healthy weight
-
Limit alcohol
-
Get vaccinated for hepatitis
-
Avoid unnecessary medications
-
Eat balanced meals
-
Exercise regularly
-
Get regular liver function tests
Your liver doesn’t complain loudly — but it deserves attention.
Conclusion
The liver is truly one of the most extraordinary organs in the human body. It regenerates, detoxifies, stores energy, balances hormones, and performs hundreds of life-saving functions every single day.
Yet, it works silently — until something goes wrong.
Understanding what makes the liver unique empowers you to take better care of it. And if severe liver disease ever occurs, consulting the best liver transplant surgeon in india can offer hope, advanced treatment, and a second chance at life.
Take care of your liver today — because it takes care of you every moment.
Frequently Asked Questions (FAQs)
1. Why is the liver considered a unique organ?
Because it can regenerate, perform over 500 functions, filter toxins, store energy, and support digestion — all at the same time.
2. Can a person live without a liver?
No. The liver is essential for survival. However, liver transplant surgery can replace a failing liver.
3. What are early warning signs of liver disease?
Early stages may show no symptoms. Later signs include fatigue, jaundice, abdominal swelling, and weight loss.
4. Is liver transplant safe in India?
Yes. With experienced transplant teams and modern facilities, outcomes are excellent, especially when treated by the best liver transplant surgeon in India.
5. How can I naturally improve my liver health?
-
Maintain a healthy weight
-
Eat balanced meals
-
Exercise regularly
-
Limit alcohol
-
Get routine health check-ups