The liver is one of the most hardworking organs in the human body. It acts like a silent superhero that filters toxins, supports digestion, stores energy, and keeps your body functioning smoothly. But what happens when this important organ becomes damaged? Thankfully, medical science has made incredible progress in recent years. Today, patients have access to some of the most advanced liver treatments that can improve quality of life and even save lives.
Whether someone is dealing with fatty liver disease, liver cirrhosis, hepatitis, liver failure, or liver cancer, modern treatment options are offering new hope every day. From robotic surgeries to liver transplants and regenerative therapies, the future of liver care looks brighter than ever.
If you or a loved one are searching for information about advanced liver treatments or looking for the best liver transplant surgeon in india, this guide will help you understand everything in simple and easy language.
1. Understanding the Liver and Its Role
The liver is situated to the left side of abdomen. It is responsible for more than 500 vital functions. Consider it the body’s natural cleansing machine. It eliminates harmful substances from blood, assists in digesting foods, store vitamins and regulates many chemical reactions within the body.
Without a healthy liver the body has to fight for survival. So, maintaining the health of your liver is crucial.
2. Common Liver Diseases
A lot of people don’t know they have liver problems until it becomes a serious condition. The most common liver ailments are:
Fatty Liver Disease
The reason for this is that fat accumulates within the intestines. It’s becoming increasingly prevalent due to diets that are unhealthy and a lack of exercise.
Hepatitis
Hepatitis is an inflammation of the liver that is caused by alcohol, viruses or autoimmune conditions.
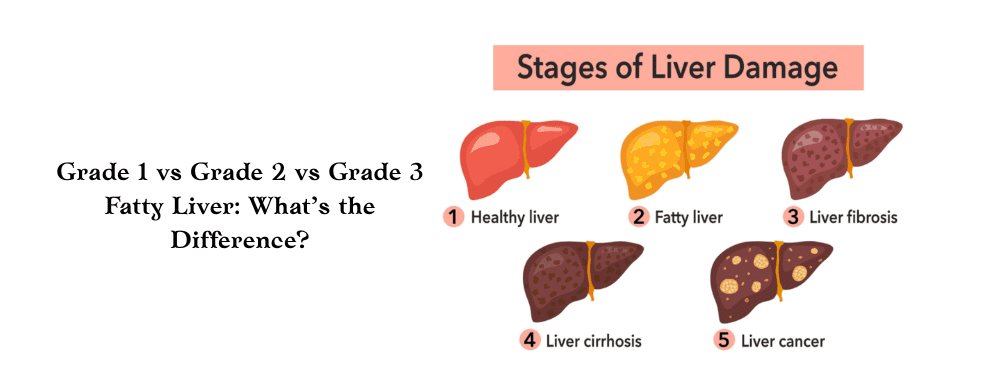
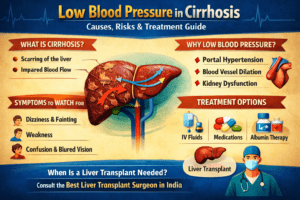
Liver Cirrhosis
Cirrhosis happens in the liver when normal tissue gets transformed into scar tissue. It may eventually cause liver failure.
Liver Cancer
Cancer of the liver can occur in patients with chronic damage to the liver.
Acute Liver Failure
It is an abrupt impairment of the liver that needs immediate medical attention.
3. Early Warning Signs of Liver Problems
The liver is often silently affected. This is why it’s important to detect symptoms in the early stages.
Common Symptoms Include:
- Eyes as well as skin (jaundice)
- Abdominal swelling
- Extreme tiredness
- Dark urine
- A loss of appetite
- Nausea and vomiting
- Itchy skin
- The loss of weight
If the symptoms persist and persist, contacting the liver specialist immediately could help to avoid serious complications.
4. Why Advanced Liver Treatment Matters
In the past, liver disorders were usually considered to be incurable in the advanced stages. Today, advances in medical technology and medical research have transformed everything.
Modern liver treatments focus on:
- The early diagnosis
- Precise treatment
- Less pain
- Faster recovery
- Greater survival rates
Modern treatments can allow patients to live longer and live longer lives.
5. Latest Diagnostic Technologies for Liver Disease
Before beginning treatment doctors must be aware of the problem thoroughly. Modern diagnostic tools can make this simpler and more precise.
FibroScan
This non-invasive test tests the stiffness of the liver and levels of fat without surgical intervention.
MRI and CT Scans
Advanced imaging allows doctors to identify cancerous tumors, scarring and damage to the liver.
Liver Function Tests
Blood tests test for proteins and enzymes in order to determine the health of your liver.
Liver Biopsy
A small portion of the tissue from the liver gets studied under the microscope.
These tools help doctors design the most effective treatment plan.
6. Advanced Medicines for Liver Conditions
Liver disease treatments have significantly improved in recent years.
Antiviral Therapy
Modern antiviral drugs can successfully combat the hepatitis B as well as C.
Immunotherapy
This treatment increases the immune system of the body to fight cancer in the liver.
Targeted Therapy
The targeted drugs target cancerous cells, while also reducing damage to healthy tissues.
Anti-Fibrotic Drugs
These medications aim to decrease the scarring of the liver in cirrhosis patients.
With the proper medication plan the majority of liver ailments are now controlled effectively.
7. Minimally Invasive Liver Surgery
Traditional open surgeries typically required large cuts as well as lengthy recovery time. Nowadays, minimally-invasive surgeries have revolutionized patient care.
Benefits of Minimally Invasive Surgery
- Smaller cuts
- Less bleeding
- Lowers pain
- Shorter hospital stay
- Faster healing
They are often used to treat liver cysts, tumors, and gallbladder-related disorders.
8. Robotic and Laparoscopic Liver Procedures
One of the latest innovations in liver health is robotic surgery.
Robotic Liver Surgery
Robotic systems enable surgeons to perform their work with astonishing precision. It’s as if they give the surgeon the ability to control a robot with superhuman precision and control.
Advantages Include:
- Higher precision
- Better safety
- Minimal scarring
- Quick recovery
Laparoscopic Liver Surgery
In this method surgeons make use of small instruments and cameras that go through small cut.
Modern techniques are becoming more popular in India’s most prestigious hospitals.
9. Liver Transplant: The Most Advanced Solution
When the liver becomes seriously damaged A liver transplant could be the only option to save your life.
The liver transplant is a procedure to replace the injured organ by a healthy one by a donation.
Presently, India is known globally for its cost-effective and efficient liver transplants that are affordable and effective. A lot of patients from all over the world visit India to get treatment by the top liver transplant surgeons in India..
Who Needs a Liver Transplant?
Patients suffering from:
- Stage-ending liver diseases
- Severe cirrhosis
- Liver failure
- Certain liver cancers
- Genetic liver disorders
may require transplantation.
10. Types of Liver Transplant Procedures
Living Donor Liver Transplant
In this process the patient is healthy and gives a small portion the liver. The liver is able to grow naturally following surgery.
Deceased Donor Liver Transplant
The liver is derived from a brain-dead person the family of whom has agreed with organ donations.
Split Liver Transplant
One donor’s liver is split into two patients, generally the child and the adult.
Why Liver Transplant Is Amazing
The liver is regenerative that means it is able to grow following surgery. It’s like nature’s self-repairing machine.
11. Recovery After Liver Treatment
The recovery process is based on the type of treatment you receive.
Post-Treatment Care Tips
- Make sure to take your medicine on time
- Make follow-up appointment
- Avoid alcohol completely
- Consume healthy food
- Keep physically active
- Maintain an appropriate weight
The majority of patients are able to get back to normal activities following the successful treatment and appropriate treatment.
12. Diet and Lifestyle Changes for Liver Health
Your lifestyle plays a major part in the recovery of your liver and prevention.
Foods That Support Liver Health
- Fruits and veggies that are fresh
- Whole grain
- Lean protein
- Seeds, nuts and nut
- Healthful fats
Avoid These Foods
- Alcohol
- Fried food
- Sweet drinks
- Processed food
- Excess salt
Exercise Regularly
Even walking for 30 minutes each day can help improve the function of your liver.
13. Choosing the Best Liver Specialist
Choosing the right doctor is among the most crucial decisions.
What to Look For
Experience
Select a doctor with vast expertise in liver transplantation and surgery.
Hospital Facilities
Modern hospitals that have ICU support and cutting-edge technology can provide better outcomes.
Success Rates
Always be sure to check the success rate of your transplant and patient feedback.
Multidisciplinary Team
A team of surgeons, hepatologists, nutritionists, and other critical health experts can improve the patient’s care.
India is home to a variety of expert liver specialists who are highly skilled Finding the most skilled liver transplant surgeon from India will significantly increase the chances of success.
14. Future Innovations in Liver Treatment
Medical science continues to develop quickly.
Stem Cell Therapy
Researchers are studying stem cells for the repair of the damaged tissue of liver.
Artificial Liver Support Systems
The machines can temporarily assist the liver’s function until it recovers or a transplant.
Gene Therapy
Scientists are developing ways to treat inherited liver diseases at the genetic level.
3D Printed Organs
Although still in the early stages 3D-printed organs may revolutionize transplantation forever.
The next phase of liver therapy is exciting and brimming with possibilities.
15. Final Thoughts
Liver diseases can be frightening But modern medicine has opened up doors that were once thought to be impossible. Modern diagnostics surgical robotics, specific drugs and liver transplantation help thousands of patients live longer and healthier lives.
The most important thing is to detect the symptoms early and prompt treatment. The inability to recognize symptoms could cause serious complications While prompt medical treatment could make all the difference.
In the event that you, or anyone you know struggles with liver issues Don’t give up the hope. Talk to a seasoned liver specialist and learn about the most recent treatments offered. With the help of the most experienced liver transplant surgeon in India modern liver treatment could be a life-saving journey.
FAQs
1. Is there a more effective cure for liver diseases?
The most modern treatment relies on the severity of the problem. Options include the use of robotic surgery as well as the targeted treatment, immunotherapy as well as liver transplantation.
2. Who is in need of an organ transplant?
People suffering from severe liver problems or advanced cirrhosis, liver cancer or other genetic liver diseases may require a liver transplant.
3. Are liver transplants beneficial in India?
Indeed, India has highly experienced specialists and modern hospitals with great rates of success with liver transplants.
4. Can the fatty liver disease be reversed?
In many instances, the fatty liver disease is treated with healthy diet exercising as well as weight loss or medical therapy.
5. Where can I find the most effective liver transplant doctor in india?
Find a surgeon who has an extensive expertise, a high rate of success and modern hospital support and positive feedback from patients.