Why International Patients Travel to India for Liver Cancer Treatment
Liver cancer is one of the most serious health conditions affecting people around the world. Hearing the words “You have liver cancer” can feel like standing in the middle of a storm with no clear direction. But today, many patients are finding hope thousands of miles away—in India.
Over the last decade, India has become a trusted destination for advanced liver cancer treatment. Patients from Africa, the Middle East, Southeast Asia, Europe, and even developed countries like the USA and the UK are choosing Indian hospitals for treatment. But why exactly are people travelling so far for healthcare?
The answer is simple: world-class doctors, modern technology, affordable costs, and high success rates.
India is home to some of the best liver transplant surgeon in India, offering advanced treatment options such as liver transplantation, targeted therapy, robotic surgery, chemotherapy, immunotherapy, and minimally invasive procedures. For many patients, treatment in India feels like getting premium healthcare without the overwhelming financial burden.
Think of it like flying business class at the price of economy. Patients receive high-quality medical care, but at a much lower cost compared to many Western countries.
In this article, we’ll explore why India has become a global hub for liver cancer treatment and what international patients can expect during their medical journey.
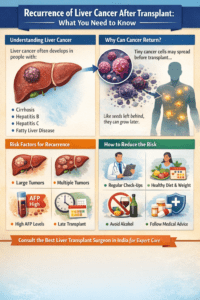
1. Understanding Liver Cancer
Liver cancer is a condition that occurs when abnormal cells multiply in the liver, uncontrollably. The liver is among the most vital organs in the body since it helps eliminate the toxins, process food, and stores energy.
The most commonly used kind of cancer in the liver can be Hepatocellular Carcinoma (HCC).
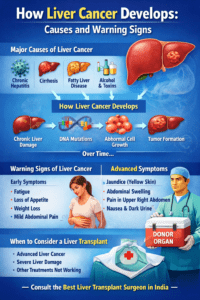
Common Symptoms of Liver Cancer
- Unexplained weight loss
- A loss of appetite
- Upper abdominal pain
- The eyes and skin are prone to yellowing (jaundice)
- Insomnia and fatigue
- Abdominal swelling
Most patients don’t show any signs in the first stages and that’s why the diagnosis of liver cancer often comes in the later stages.
2. Why Liver Cancer Cases Are Increasing
Liver cancer incidences are rising across the globe. Numerous health and lifestyle causes are behind the increase.
Major Causes Include
- Hepatitis B as well as C-related infections
- Fat-liver disease
- Excessive alcohol use
- Obesity
- Diabetes
- Smoking
In a number of nations, access to the latest liver treatment is not available or extremely costly. This is among the primary reasons that patients are forced to seek treatments in other countries.
3. Why India Is a Global Healthcare Destination
India has earned a solid reputation for medical tourism. Each year, thousands of patients from around the world travel to India to receive complex treatments, such as liver cancer care.
Why Patients Prefer India
- Highly skilled and experienced doctors
- Hospitals internationally accredited
- Affordable healthcare
- Advanced medical equipment
- Medical staff who speak English
- Faster treatment scheduling
Many Indian hospitals follow international health standards and offer care that is comparable to international benchmarks for quality.
Cities such as Delhi, Mumbai, Chennai, Hyderabad, and Bangalore are famous for their modern centres for liver treatments.
4. Affordable Treatment Costs in India
One of the major reasons that international travelers visit India is the cost.
In nations like those of the USA and the UK treatments for cancer of the liver is expensive. The procedure of a liver transplant alone could cost millions of dollars.
Cost Comparison
| Treatment | Approximate Cost in USA | Approximate Cost in India |
|---|---|---|
| Liver Transplant | $300,000+ | $30,000-$50,000 |
| Chemotherapy | Very High | Much Lower |
| Radiofrequency Ablation | Expensive | Affordable |
| Immunotherapy | Costly | Budget-Friendly |
Patients could save as much as 60-80% on their treatment expenses while still receiving high-quality medical treatment.
If you have a family that is already emotionally overwhelmed and financially stressed, this financial relief can help a lot.
5. Access to the Best Liver Specialists
India is renowned as having the most skilled liver surgeons and oncologists around the globe.
The liver transplant specialist in india usually includes:
- International training
- Experience gained from years of surgery
- Expertise in complicated liver surgery
- High success rates
- Experience in dealing with international patients
A lot of surgeons in India carry out thousands of liver transplants each year, which gives them a the expertise needed to handle difficult cases.
Why Experience Matters
Liver surgery can be extremely delicate. It’s just like fixing the engine of an aircraft the precision and experience are essential.
Doctors with experience increase the odds of a successful treatment and speedier recovery.
6. Advanced Technology and Modern Hospitals
The top hospitals in India are outfitted with the latest medical technology that allows for precise diagnostics and treatments.
Modern Facilities Often Include
- Robotic surgical systems
- PET-CT scans
- Advanced imaging and MRI
- Therapy with a specific goal
- Immunotherapy
- Minimally surgery that is not invasive
- Advanced ICU medical care
These techniques help doctors identify cancer earlier and develop more effective treatment strategies.
A lot of hospitals have liver transplantation units that have specialized teams available 24 hours a day.
7. High Success Rate of Liver Transplants
Transplantation of the liver is usually the most effective treatment option for cases of advanced liver cancer.
India has seen astounding success rates for liver transplant operation. The top hospitals have survival rates that are comparable to international standards.
Why Success Rates Are High
- Teams of skilled surgeons
- Advanced post-operative care
- Improved control of infections
- Individualized recovery plans for each client
- Regularly-scheduled monitoring
Many patients find that an organ transplant is an opportunity to live again.
8. Personalized Treatment Plans
No two liver cancer patients are alike.
Indian doctors typically create custom treatment plans that are based on:
- Cancer stage
- Patient age
- Overall general health
- Condition of the liver
- Medical background
Treatment Options May Include
- Surgery
- Transplantation of the liver
- Chemotherapy
- Therapy with radiation
- Immunotherapy
- Therapy with a specific goal
- Procedures for ablation
This individualized approach can improve results and helps reduce unnecessary treatments.
9. Short Waiting Time for Treatment
In certain nations, patients might have to be waiting for weeks, or even months for appointments with a specialist or procedures.
India provides much quicker access to treatments.
Benefits of Faster Treatment
- Early intervention
- The disease is less likely to progress
- Patients are less stressed and have less stress
- Better survival chances
In the case of cancer patients, timing is vitally important. The speed of treatment may be the difference between a cure or worsening the illness.
10. Medical Visa and International Patient Support
India has made it easier for medical travel.
Many hospitals offer complete international support for patients.
Support Services Include
- Visa assistance
- Airport pickup at the airport
- Hotel arrangements
- Language interpreters
- Information on exchange rates
- Diet planning
- Follow-up coordination
This eases the process for the patients and their families.
Hospitals recognize that patients from abroad are far from their homes and can often offer practical and emotional support as well.
11. Comfort and Hospitality for Foreign Patients
Indian culture is renowned for its warmth and hospitality. International patients are often welcomed and treated with respect throughout their stay.
Why Patients Feel Comfortable
- Hospital staff are friendly and welcoming.
- Affordable accommodations
- Food items from around the world are readily available.
- Cultural sensitivity
- Family-centered care
Some hospitals even have areas and coordinators specifically for international patients.
Many families find this supportive environment eases anxiety when undergoing treatments.
12. Popular Liver Cancer Treatments in India
India provides a broad range of treatments for cancers of the liver that are based on international medical standards.
Surgical Removal
Doctors will remove the cancerous section of the liver, if it is discovered in the early stages of.
Liver Transplant
The damaged liver is replaced by an organ that is healthy.
Chemotherapy
Drugs are used to kill cancerous cells.
Targeted Therapy
These medications specifically target cancer cells while also protecting healthy tissues.
Immunotherapy
This treatment aids the immune system fight against cancer naturally.
Radiofrequency Ablation
Energy from heat destroys cancerous tumors.
Patients usually receive a mix of treatments to achieve the most effective outcomes.
13. How to Choose the Right Hospital and Surgeon
The choice of the best hospital is among the most crucial decisions.
Things to Check Before Choosing
- The experience of a doctor
- Accreditation of hospitals
- Rate of success
- Patient reviews
- Technology is available
- International patient care services
It’s always good to talk about:
- Treatment options
- Expected outcomes
- Time to recover
- Risks and complication
- Total cost
Research can help patients make confident decisions based on facts.
14. Recovery and Follow-Up Care
The recovery process following treatment for cancer of the liver requires patience and a proper treatment.
Important Recovery Tips
- Take the advice of a doctor.
- Eat a healthy diet
- Beware of smoking and drinking alcohol.
- Make sure you take your medicine frequently
- Follow-up appointments should be scheduled.
A lot of Indian hospitals also offer online follow-up consultations following patients’ have returned home.
This guarantees that you will receive medical advice regardless of where you are in the world.
15. Final Thoughts
India is now one of the most sought-after locations for treatment of liver cancer — and with reason.
Patients who travel to India typically find a potent combination of:
- Accessible treatment
- Experts with years of experience
- Modern hospitals
- Personalized care
- Access to surgery faster
If you’re battling liver cancer the importance of hope is just as much as the treatment. India has both.
A presence by the liver transplant surgeons in India and internationally renowned hospitals provides patients with confidence in an extremely challenging experiences of their lives.
Going abroad for treatment can appear daunting at first, however for a lot of patients, it’s the experience that alters and sometimes even saves their lives.
FAQs
1. Why do international patients go to India for treatment of liver cancer?
International tourists opt for India due to the low cost and experienced doctors, as well as the latest technology, and top-quality hospitals.
2. Does treatment for liver cancer in India secure?
Yes Many Indian hospitals adhere to internationally accepted safety guidelines and employ highly skilled liver specialists who have excellent rate of success.
3. How much will treatment for liver cancer price in India?
The price varies based on the type of treatment, the hospital, and patient’s health however, it is usually less expensive than Western countries.
4. Are foreign patients able to obtain medical permits for India?
Indeed, India offers medical visas for patients from abroad Numerous hospitals can assist in the process of obtaining visas.
5. Where can I find the top surgeon for liver transplants in india?
It is possible to research accreditations for hospitals and doctor experiences, as well as patients’ reviews as well as success rates and international patient services prior to making a final decision.