Introduction
Have you ever thought about how much work your liver does for you– every single day? It quietly filters toxins, processes nutrients, and keeps your body running like a well-oiled machine. But what happens when this silent hero starts to fail?
Liver disease often develops slowly, without loud warning signs. By the time symptoms appear, the damage may already be serious. The tricky part? Many causes are hidden in everyday habits we barely notice.
Explore the liver transplant procedure, cost, recovery, and how to choose the best liver transplant surgeon in india
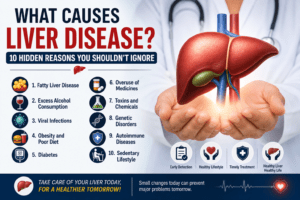
Let’s uncover the 10 hidden reasons behind liver disease— because knowing them early can literally save your life.
What is Liver Disease?
Liver disease refers to any condition that damages the liver and affects its ability to function properly. Think of your liver as a water filter— if it gets clogged or damaged, toxins start building up in your body.
There are many types, including fatty liver, hepatitis, cirrhosis, and liver cancer. The causes vary, but the result is the same: reduced liver function.
Why Understanding Causes Matters
Here’s the reality– most liver diseases are preventable.
Understanding what causes liver damage helps you:
- Take early action
- Avoid risky habits
- Seek treatment before complications arise
Ignoring the causes is like ignoring a small crack in a dam– it may look harmless at first, but it can lead to a major breakdown.
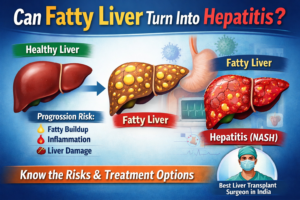
Hidden Cause # 1: Fatty Liver Disease
Non-alcoholic fatty liver disease (NAFLD) is becoming alarmingly common, especially in India.
Why it happens
- Excess fat builds up in liver cells
- Often linked to unhealthy diet
Why it’s dangerous
It usually has no symptoms in early stages but can progress to cirrhosis.
Hidden Cause # 2: Excess Alcohol Consumption
We all know alcohol can harm the liver– but do we really understand how much is too much?
What happens inside your body
Alcohol is processed by the liver. Over time, it causes:
- Inflammation
- Fat accumulation
- Permanent damage
The hidden danger
Even moderate drinking over years can silently damage your liver.
Hidden Cause # 3: Viral Infections
Hepatitis B and C are major contributors to liver disease.
How it spreads
- Contaminated blood
- Unsafe injections
- Unprotected contact
Why it’s risky
These infections can remain silent for years while slowly damaging the liver.
Hidden Cause # 4: Obesity and Poor Diet
Your daily food choices matter more than you think.
Key triggers
- Junk food
- Sugary drinks
- High-fat meals
Impact
Leads to fat buildup in the liver, increasing the risk of inflammation and damage.
Hidden Cause # 5: Diabetes
If you have diabetes, your liver is already under stress.
Connection
High blood sugar levels lead to:
- Fat storage in liver
- Increased inflammation
What to watch
Many people with diabetes develop fatty liver without knowing it.
Hidden Cause # 6: Overuse of Medicines
Yes, even common medicines can harm your liver.
Examples
- Painkillers
- Herbal supplements
- Over-the-counter drugs
Why it’s dangerous
Excessive or long-term use can cause drug-induced liver injury.
Hidden Cause # 7: Toxins and Chemicals
Exposure to harmful chemicals is often overlooked.
Sources
- Industrial chemicals
- Pesticides
- Contaminated food
Effect
These toxins damage liver cells and interfere with normal function.
Hidden Cause # 8: Genetic Disorders
Some people inherit liver conditions without realizing it.
Examples
- Hemochromatosis (iron overload)
- Wilson’s disease (copper buildup)
Why it matters
These conditions can silently damage the liver over time.
Hidden Cause # 9: Autoimmune Diseases
Sometimes, your immune system turns against your own liver.
What happens
The body mistakenly attacks liver cells, causing inflammation.
Conditions include
- Autoimmune hepatitis
- Primary biliary cirrhosis
Hidden Cause # 10: Sedentary Lifestyle
A lack of physical activity can slowly harm your liver.
Why it’s risky
- Slows metabolism
- Increases fat storage
Simple truth
Sitting all day is just as harmful as eating unhealthy food.
Early Signs You Shouldn’t Ignore
Liver disease doesn’t always shout– it whispers.
Watch out for:
- Fatigue
- Yellowing of skin (jaundice)
- Abdominal pain
- Loss of appetite
- Swelling in legs
If you notice these signs, don’t ignore them.
When to See a Specialist
If symptoms persist or tests show liver abnormalities, it’s time to consult an expert.
Why early consultation matters
- Prevents severe damage
- Improves treatment outcomes
- Avoids complications like cirrhosis
In advanced cases, consulting the best liver transplant surgeon in india can be life-saving.
Conclusion
Your liver works tirelessly– often without appreciation. But the truth is, many of us unknowingly put it at risk every day.
From unhealthy eating habits to silent infections and even medications, the causes of liver disease are often hidden in plain sight.
The good news? You have the power to protect your liver. Small lifestyle changes, regular check-ups, and early action can make a huge difference.
Think of your liver as your body’s silent guardian— take care of it, and it will take care of you.
FAQs
1. What is the most common cause of liver disease?
The most common cause is fatty liver disease, often linked to poor diet and lack of exercise.
2. Can liver disease be reversed?
Yes, in early stages, lifestyle changes and treatment can reverse or control liver damage.
3. How do I know if my liver is unhealthy?
Symptoms like fatigue, jaundice, and abdominal discomfort may indicate liver problems. Blood tests can confirm it.
4. Is alcohol the only cause of liver disease?
No, liver disease can also result from infections, obesity, diabetes, medications, and genetic factors.
5. When is a liver transplant needed?
A liver transplant is required when the liver is severely damaged and cannot function properly despite treatment.