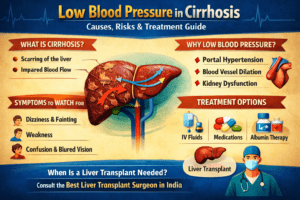
Your liver is among the most demanding organs of your body. It removes toxins, aids in digestive function, and stores nutrition and aids in maintaining general health. But what happens when your liver begins to develop scar tissue as time passes? This is known as the liver fibrosis and can slowly progress, without any obvious warning indicators.
Imagine your liver as it’s a sponge. Healthy sponges are soft and flexible, and efficient. However, if you damage it repeatedly it, it becomes rigid and hard. Liver fibrosis functions similarly. The constant trauma to the liver causes scar tissue to grow and makes it hard for your liver’s function to be normally.
The positive side? Liver fibrosis is often controlled, slowed down and even reversed if it is detected early. Knowing the symptoms can allow you to safeguard your liver and prevent serious complications such as cirrhosis or liver failure.
Understand liver fibrosis, scar tissue progression, symptoms, diagnosis, and treatment options. Learn when to consult the best liver transplant surgeon in india for advanced liver care and better long-term health outcomes.
1. What Is Liver Fibrosis?
The condition known as liver fibrosis is the growth of scar tissue in the liver as a result of frequent injury or inflammation. The liver attempts to heal itself following injury however, over time this process of healing creates fibrous tissue.
Scar tissue isn’t like the healthy tissue of your liver. It restricts blood flow and can interfere with normal function of the liver. If fibrosis is persistent for long periods it could eventually cause the condition known as cirrhosis which is an advanced form of and irreparable liver scarring.
Fibrosis by itself isn’t an illness. It is instead the result of liver damage due to alcohol, infections and fatty liver disease or other ailments.
2. How Scar Tissue Forms in the Liver
When the liver is damaged the liver’s cells are activated for repair. In this process collagen and other fibers accumulate within the liver.
The liver will continue to function normally despite small scarring. However, repeated trauma creates scar tissue. The healthy liver structure gets deformed.
Imagine patching up cracks repeatedly in the wall. After some repairs it is will no longer look or function in the same way. It’s similar to the way fibrosis alters the liver over time.
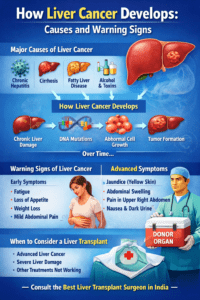
3. Common Causes of Liver Fibrosis
A variety of health issues and lifestyle choices can harm the liver, causing the development of fibrosis.
Chronic Hepatitis B and C
Viral Hepatitis can cause chronic inflammation that eventually causes scarring of the liver.
Fatty Liver Disease
Non-alcoholic fat liver illness (NAFLD) becomes more prevalent due to diabetes, obesity and a inadequate diet.
Alcohol-Related Liver Disease
The consumption of alcohol is among of the most common reasons for liver problems in the world.
Autoimmune Liver Diseases
Sometimes, the body’s immune system targets liver cells through making a mistake.
Certain Medications and Toxins
Exposure to chemicals that are harmful for long periods or the misuse of medications can harm the liver.
Genetic Disorders
The inherited conditions like hemochromatosis and Wilson’s disease can be a contributing factor to fibrosis.
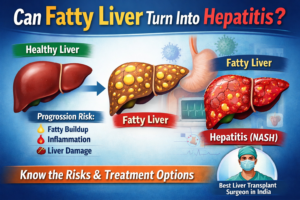
4. Stages of Liver Fibrosis
Doctors typically classify fibrosis in stages that range from F0 up to F4.
| Stage | Description |
|---|---|
| F0 | No Fibrosis |
| F1 | Scarring that is mild |
| F2 | Moderate Fibrosis |
| F3 | Fibrosis severe |
| F4 | Cirrhosis |
The higher the level the stage, the more damage to the liver.
Why Staging Matters
Knowing the stage can help doctors choose the most appropriate treatment strategy and track the progress of the disease.
5. Early Warning Signs and Symptoms
One of the most difficult issues in liver fibrosis often it does not cause any symptoms until the beginning stages.
As the condition deteriorates the possibility of:
- Fatigue
- Weakness
- Appetit loss
- Nausea
- Abdominal discomfort
- Unexplained loss of weight
Acute fibrosis or cirrhosis could result in:
- Jaundice
- Leg swelling
- Fluid accumulation inside the abdomen
- Confusion
- Easy bruising
Since symptoms can develop late due to the fact that symptoms may not be apparent until later, regular health checks are crucial for those who are who are at high risk.
6. How Doctors Diagnose Liver Fibrosis
A variety of tests can help determine if you have the presence of liver fibrosis. There are several tests that can help identify liver.
Blood Tests
Tests for liver function may identify liver damage or inflammation.
Imaging Tests
Ultrasounds, CT scans, and MRI scans are used to evaluate the liver structure.
FibroScan
This test, which is painless, determines stiffness in the liver. It is widely used today.
Liver Biopsy
In some instances doctors will remove a tiny tissue sample to conduct a thorough exam.
The early diagnosis lets doctors begin treatment before serious damage is caused.
7. Can Liver Fibrosis Be Reversed?
This is among the most frequent questions people are asked.
The good news is that Early-stage liver fibrosis in the beginning can occasionally improve or even reverse when the root causes are addressed.
For instance:
- The cessation of alcohol consumption can aid in healing the liver.
- The treatment of hepatitis infections can help reduce inflammation.
- Losing weight can help aid in the treatment of the severity of fatty liver disease.
However advanced fibrosis and cirrhosis are harder for a complete reverse.
8. Treatment Options for Liver Fibrosis
There is no one medicine that can completely treat liver fibrosis However, many treatments may stop or slow the progression.
Treating the Underlying Cause
Doctors are focused on treating the conditions that cause liver damage.
Examples Include:
- Antiviral medications for Hepatitis
- Management of diabetes
- Weight loss
- Beware of the consumption of alcohol
Medications
Certain medicines can reduce inflammation and safeguard liver cells.
Regular Monitoring
Patients frequently require routine blood tests and scans to monitor liver health.
Advanced Care
Patients with severe liver diseases might require specialized care by the top liver transplant surgeons in India in the event that liver function decreases dramatically.
9. Lifestyle Changes That Support Liver Health
A healthy lifestyle can have a significant impact on.
Eat a Balanced Diet
Concentrate on:
- Fruits and vegetables
- Whole grains
- Lean protein
- Healthy fats
Avoid:
- Foods processed for processing
- Drinks with sugary substances
- Salt in excess
Maintain a Healthy Weight
Obesity can increase the risk of developing fatty liver disease.
Avoid Alcohol
Even tiny amounts of alcohol can cause the damage to the liver in certain patients.
Exercise Regularly
Physical activity can improve the metabolic rate and reduce fat in the liver.
Stay Hydrated
Drinking enough fluids can improve the overall health of your body.
10. The Link Between Fibrosis and Cirrhosis
It is not the case that everyone who has fibrosis develops cirrhosis. However, chronic liver damage can raise the chance.
Cirrhosis is a condition that occurs when scar tissue grows and permanently interferes with the liver’s function.
The complications could include:
- Internal bleeding
- Infections
- Liver failure
- Hypertension at the portal
The the treatment is focused on preventing the development of complications while preserving the remaining liver function.
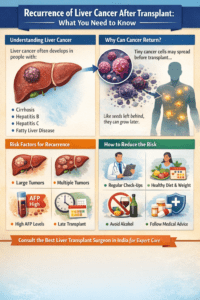
11. Liver Fibrosis and Liver Cancer Risk
The presence of advanced fibrosis and cirrhosis increases the risk of developing liver cancer.
People suffering from chronic hepatitis and cirrhosis usually require regular screening tests like:
- Ultrasounds
- AFP blood tests
- The MRI scans
Early detection significantly improves the chance of success in treatment.
12. When Is a Liver Transplant Needed?
A liver transplant can be essential if the liver is unable to no longer fulfill its essential duties.
Signs That a Transplant May Be Required
- Cirrhosis severe
- Recurring fluid buildup
- Liver failure
- Liver cancer in certain instances
Selecting a reputable medical team is crucial. A lot of patients seek advice from the top liver transplant surgeons in India to receive the most advanced treatment and evaluation of transplants.
India is now a renowned location for liver transplants due to highly skilled surgeons and modern medical infrastructure.
13. Importance of Early Detection
Early detection is a great way to increase the chances of success.
The most at-risk people need to have regular liver checks for the following reasons:
- Hepatitis-infected people
- People suffering from diabetes
- Heavy alcohol users
- Patients with obesity or the fatty liver disease
The early detection of fibrosis can keep liver damage from becoming irreparable.
14. Tips to Prevent Liver Fibrosis
It is better to prevent than cure.
Get Vaccinated
Hepatitis vaccinations A and B to protect the liver.
Practice Safe Hygiene
Be wary of sharing needles or personal items that can transmit infections.
Limit Alcohol Intake
The reduction in alcohol consumption reduces stress on the liver.
Control Diabetes and Cholesterol
Monitoring metabolic health can protect the liver.
Avoid Self-Medication
Certain medicines and supplements may harm the liver when used incorrectly.
Schedule Regular Health Checkups
Monitoring routinely helps to identify issues before they get more serious.
15. Final Thoughts
Liver fibrosis can sound scary but knowing the cause can be the initial step to safeguarding your health. The liver is extremely resilient and is able to heal provided the right care.
The most important thing is to take action as soon as possible. If the reason is the hepatitis virus, fatty liver disease or alcohol consumption, or other condition, prompt treatment may slow or reverse liver damage in a lot of instances.
If you or someone close to you is suffering from liver issues for a long time Do not overlook the warning indicators. Seek out a specialist who is qualified and adhere to a healthy life style, and seek professional assistance when required. For more serious cases, contacting the top liver transplant surgeons in India will help patients consider the best options for life-saving treatments and enhance the long-term outcome.
FAQs
1. What is the primary reason for liver fibrosis?
The most frequent causes are the hepatitis infection as well as fatty liver disease. excessive alcohol consumption and chronic inflammation of the liver.
2. Does liver fibrosis disappear completely?
Early-stage fibrosis can be reversed or improved when the causes are treated promptly.
3. Is liver fibrosis the exact same as cirrhosis?
No. Fibrosis can be characterized as mild or early scarring, while cirrhosis can be severe and has extensive liver damage.
4. How long will the progression of liver fibrosis last?
The course of treatment varies from one person to the next individual. Certain people will have severe fibrosis before the age of but others can require several decades.
5. When should one consult a specialist in the field of liver?
Anyone who has chronic liver problems, hepatitis the fatty liver disease and abnormal tests for the liver, should seek out a doctor for a medical evaluation.